Did You Know That You Can Practice Yoga Therapy to Ease Prostatitis?
Yoga is a form of exercise that utilizes movement for strength and flexibility, along with breathwork and mindfulness for reduction of stress and tension. Yoga has long been used therapeutically for a variety of neuromuscular, immunological, psychological, and pain disorders. It has also been linked to improvements in body awareness, improved cognition, flexibility and strength, as well as physiology (reducing stress hormones, improving cardiac function) (Schmalzl et al, 2015).
Prostatitis and Male Pelvic Pain
Chronic prostatitis, nonbacterial prostatitis, and chronic pelvic pain are all related conditions which negatively affect quality of life for the men who suffer from them. Symptoms vary, but are often described as a “headache in the pelvis” with pain symptoms affecting urinary and sexual function. The pain is real and their negative affects on quality of life are real as well. The pain caused by nonbacterial prostatitis can be disabling, preventing participation in valued activities and causing isolation and depression.
According to Harvard Medical School, prostatitis accounts for about 1.8 million visits to the doctor’s office in the United States each year. Between 9% to 16% of men of all ages experience prostatitis. About 90% of these instances cannot be tied to an active bacterial infection. Prostatitis affects men of all ages, unlike benign prostatic hyperplasia (BPH) and prostate cancer, which predominantly affect older men.
Yoga, Pelvic Floor Dysfunction, and Chronic Pain
Yoga can help both strengthen and increase flexibility of the pelvic floor muscles and surrounding musculature to better function and treat issues such as pain with urination, pain with ejaculation, and pain with bowel movements.
Research has shown to be a viable tool in chronic pain management. Yoga practice has been tied to a decrease in pain in practitioners. Gupta et al. suggested that yoga therapy is part of an ideal model of care for interstitial cystitis/painful bladder sydrome. The symptoms of IC and painful bladder syndrome are similar to that of prostatitis, and men tend to be diagnosed with the latter, despite them sharing similar musculoskeletal findings in the pelvic floor muscles.
An article in the Journal of Exercise Rehabilitation recommends yoga as an intervention for pelvic floor dysfunction and pelvic pain (Chung, K. J., Han, A. N. Y., & Kim, K. H. (2015).
As a pelvic floor therapists and a registered yoga teachers, we have seen the power of gentle yoga poses to help stretch and lengthen the muscles and tissues in the abdomen, pelvis, low back, and hips during painful flareups and the reduction of pain over time.
Here are a few yoga poses to try if you are dealing with prostatitis-related or chronic pelvic pain.
What you will need:
- Pants you can stretch in
- An empty wall
- Yoga mat or folded blanket, rug, etc. for padding
- A pillow or bolster
1. Deep Breathing

It is found that those with chronic pain often often present in our office with short and shallow breathing. This type of breathing adds tension to the diaphragm, abdomen, and pelvic floor. Relearning how to breath deeply is a profound way to start unraveling the tension inside the body. This tension is often held in the space between the ribs, neck, shoulders, low back, belly and pelvic floor. Studies also show that diaphragmatic breathing can help the body break the pain cycle, thereby reducing pain and chronic pain (Roditi & Robinson, 2011).
Deep breathing can be practiced anywhere: while stuck in a traffic jam, waiting in line at the grocery store, or at night before you go to bed. The importance of breathing is so important, Apple includes it as an App on the Apple Watch, and other great breathing apps are becoming more and more popular in the App Store (we like Breathing Zone). To help improve rib mobility and reduce pain in the areas listed above, try this:
- Lie on your back. Knees can be bent with feet flat on the floor, or knees can be propped up on a pillow, wedge or bolster.
- Place one hand over the heart and one over the belly button.
- Inhale through the nose and feel both hands rise as you inhale. Ribs are expanding, belly is also expanding, even the back of the body expands into the mat. Exhale gently and slowly, either through pursed lips or the nose. The air is slowly escaping as if you poked a hole in a tire with a needle and the air slowly passes out. The goal is to elongate the exhale, so that it is longer than the inhale.
- When the breath has been fully exhaled, pause for a second or two before beginning the breath cycle again, with another inhale. After you have exhaled wait a couple of seconds until you inhale again. Continue to breathing for 5-10 minutes
2. Hamstring Stretch at the Wall

- Lie down comfortably on floor with both legs against the wall, feet towards the sky.
- Keep knees straight and pull toes down towards your face
- Relax your low back, pelvis and shoulders.
- Keep your knees soft, NOT Locked.
- Keep your glutes and low back flat on floor.
- Breathe deeply throughout the stretch.
3. Abductor Stretch at the Wall

- Lie down comfortably on floor or bed with both legs on wall, as in the hamstring stretch (above).
- Rotate toes and hips outward and gently allow legs to slide out into a “V” shape.
- Relax your low back and shoulders.
- Keep knees soft, NOT Locked.
- Keep your glutes and low back flat on floor.
- Breathe deeply throughout the stretch.
4. Hip & Buttock Stretch

- Lie down comfortably on floor or bed with both legs on wall, as in the hamstring stretch (above).
- Place one ankle on opposite thigh.
- Slide opposite foot down wall until stretch is felt in hip/glute.
- Place gentle pressure with hand on knee (as seen in picture).
- Breathe deeply throughout the stretch.
5. Groin Stretch/Pelvic Floor Relax Position
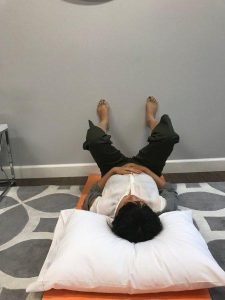
- Start in hamstring stretch position, bring knees to chest, feet flat on the wall.
- Do deep breathing and allow the pelvic floor muscles to sink into the mat, relaxing the muscles.
- Rest here for 60 seconds, and focus on your deep breathing and pelvic floor relaxation.
6. Hip Flexor Stretch/Runner’s Lunge

- Begin in a kneeling position on a mat (you may have a towel or blanket under the knees)
- Step one foot forwards.
- Lean hip points forward, feeling a stretch down your quad in into the hip flexor.
- Maintain a neutral pelvic position.
- If you are feeling balanced, reach both arms towards the sky, spreading the collarbones towards the ceiling.
- You can rest here for 60 seconds, and focus on your deep breathing and pelvic floor relaxation.
7. Cobra Pose

- Lie on your belly and spread your hands under the shoulders. Elbows hug in towards the body, in line with the nipples.
- Press the tops of the feet, thighs and the pelvis into the floor.
- On an inhalation, use arms to support you as you lift the chest off the floor. Do not go too high, 4-10 inches.
- Firm the glute muscles, without clenching the cheeks together. Bring the belly button to spine, engaging the low belly to support the low back.
- Breathe long and deeply for 1 minute.
8. Child’s Pose

- Start in a quadraped (hands and knees) position
- Sit back on your heels and curl forwards, bringing your forehead to the mat
- Reach your arms forward on the mat
- Modification: Try this position with a pillow or a bolster supporting the glutes and/or chest. A pillow under your thighs also works if you are experiencing knee pain.
- Rest here for 60 seconds, and focus on your deep breathing and pelvic floor relaxation
Resources:
*Anderson RU, Wise D, Sawyer T, Chan C. (2005). Integration of Myofascial Trigger Point Release and Paradoxical Relaxation Training Treatment of Chronic Pelvic Pain in Men. Journal of Urology;174:155–60. PMID: 15947608.
*FitzGerald MP, Anderson RU, Potts J, et al. (2009). Randomized Multicenter Feasibility Trial of Myofascial Physical Therapy for the Treatment of Urological Chronic Pelvic Pain Syndromes. Journal of Urology;182:570–80. PMID: 19535099.
*O’Leary, M. (2011).Treating prostatitis: Any cause for optimism?. Harvard Medical School Health Publications: Prostate Knowledge. Accessed at: https://www.harvardprostateknowledge.org/treating-prostatitis-any-cause-for-optimism
*Chung, K. J., Han, A. N. Y., & Kim, K. H. (2015). Recommendations to the primary care practitioners and the patients for managing pelvic pain, especially in painful bladder syndrome for early and better prognosis.Journal of Exercise Rehabilitation, 11(5), 251–254. https://doi.org/10.12965/jer.150226
*Curtis, K., Weinrib, A., & Katz, J. (2012). Systematic Review of Yoga for Pregnant Women: Current Status and Future Directions. Evidence-Based Complementary and Alternative Medicine : eCAM, 2012, 715942.https://doi.org/10.1155/2012/715942
*Gupta, P., Gaines, N., Sirls, L. T., & Peters, K. M. (2015). A multidisciplinary approach to the evaluation and management of interstitial cystitis/bladder pain syndrome: an ideal model of care. Translational Andrology and Urology, 4(6), 611–619. https://doi.org/10.3978/j.issn.2223-4683.2015.10.10
Huang, A. J., Jenny, H. E., Chesney, M. A., Schembri, M., & Subak, L. L. (2014). A Group-Based Yoga Therapy Intervention for Urinary Incontinence in Women: A Pilot Randomized Trial. Female Pelvic Medicine & Reconstructive Surgery, 20(3), 147–154.https://doi.org/10.1097/SPV.0000000000000072
Schmalzl, L., Powers, C., & Henje Blom, E. (2015). Neurophysiological and neurocognitive mechanisms underlying the effects of yoga-based practices: towards a comprehensive theoretical framework. Frontiers in Human Neuroscience, 9, 235.https://doi.org/10.3389/fnhum.2015.00235