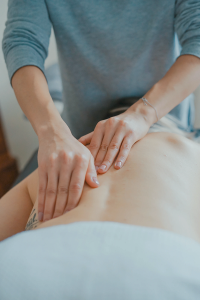
It has long been recognized in the Pelvic Physical Therapy World that there is a connection between urinary incontinence and low back pain.
Clinically, we often see patients that come in with both symptoms. How common is urinary incontinence among people also affected by low back pain? What comes first, the urinary incontinence or the back pain? What causes this?
In a recent systematic review, a positive association of 83% was found between urinary incontinence and low back pain or pelvic girdle pain. Pelvic girdle pain is defined as the area below the low back and below the abdomen (gluteal region in the back and pubic bone in the front). The strength of this correlation depends on many factors such as type of urinary incontinence, pain severity, and length of pain.
The relationship between urinary incontinence and low back pain is seen equally in both men and women and can be applied to all folks. Low levels of low back pain were mostly associated with both, stress urinary incontinence (SUI) and mixed urinary incontinence (MUI). Whereas high levels of low back pain were associated more with urge urinary incontinence. Based on one study by Stockil et al., SUI was seen more often with sudden onset pains than with chronic pain. Unfortunately, their sample of patients was limited, consisting mostly of young women who have never given birth. To measure the correlation more accurately, studies involving a broader population will need to be conducted.
What causes the link between urinary incontinence and low back pain?
One theory that could contribute to the development of both urinary incontinence and lumbopelvic pain is decreased coordination of the abdominal muscles and the pelvic floor muscles.
A combined activation of the abdominal wall muscles, diaphragm, pelvic floor muscles (PFM), and muscles of the spine is necessary to ensure the control of basic functions such as continence, breathing, gastrointestinal function, and spinal stability” (Sapsford., 2001 Hodges., 2000).
Several studies have found that both the transversus abdominis muscle (TRA) and the pelvic floor muscles must engage before movement to stabilize the spine and pelvis (Hodges et al., 2000, 2007 Stocki et al., 2018). Without this anticipatory activation, the development of low back pain, pelvic girdle pain, and/or stress urinary incontinence can result. Several studies displayed similar findings regarding pelvic floor muscle function in patients with urinary incontinence and low back pain compared to a healthy population. Women with urinary incontinence and low back pain present with reduced muscle endurance, a delayed automatic pelvic floor muscle contraction, altered length of the pelvic muscles, and poor coordination between the pelvic floor and abdominal muscles (Sjödahl et al., 2016 Stuge., 2006 Smith., 2007 Devreese., 2004).
Treating urinary incontinence and low back pain
Clinicians should be aware of the strong link between urinary incontinence and back/pelvic girdle pain. They must screen for incontinence during the evaluation and refer out to providers that are specialized to treat pelvic floor dysfunctions. The effect of pelvic floor muscle therapy in subjects with lumbopelvic pain has been studied in several clinical trials (Ayod., 2019 Teymuri., 2012 Ghaderi., 2016 Taylor., 2018). Pelvic floor therapy has been found to improve not only pelvic floor dysfunction symptoms but also pain and disability related to PGP and LBP.
If you are experiencing back or pelvic girdle pain and have not found relief, or are also experiencing urinary incontinence, pain with intercourse, pain with bowel movements, or pelvic pain; make an appointment with a pelvic health therapist that is strong with their orthopedic skills, too, for an evaluation. Contact us here for an in-office or telehealth session in California (or virtual consultation worldwide).
References
Bertuit, Jeanne, et al. “Relationship between Urinary Incontinence and Back or Pelvic Girdle Pain: a Systematic Review with Meta-Analysis.” International Urogynecology Journal, vol. 32, no. 5, 2021, pp. 1073–1086., doi:10.1007/s00192-020-04670-1.
Sapsford RR, Hodges PW, Richardson CA, et al. Co-activation of the abdominal and pelvic floor muscles during voluntary exercises. Neurourol Urodyn. 2001;20:31–42.
Stockil L, Thompson J, Briffa K, et al. Urogenital symptoms: prevalence, bother, associations and impact in 22 year-old women of the Raine study. Int Urogynecol J. 2018;29:1807–15. https://doi.org/ 10.1007/s00192-018-3639-x.
Hodges PW, Sapsford R, Pengel LHM. Postural and respiratory functions of the pelvic floor muscles. Neurourol Urodyn. 2007;26:362–71. https://doi.org/10.1002/nau.20232
Hodges PW, Cresswell AG, Daggfeldt K, Thorstensson A. Threedimensional preparatory trunk motion precedes asymmetrical upperlimb movement. Gait Posture. 2000;11:92–101.11. Hodges PW, Richardson CA. Inefficient muscular stabilization ofthe lumbar spine associated with low back pain. A motor controlevaluation of transversus abdominis. Spine. 1996;21(22):2640–50.https://doi.org/10.1097/00007632-199611150-00014
Devreese A, Staes F, De Weerdt W, et al. Clinical evaluation of pelvic floor muscle function in continent and incontinent women. Neurourol Urodyn. 2004;23(3):190–7.
https://doi.org/10.1002/nau. 20018.
Smith MD, Coppieters MW, Hodges PW. Postural response of the pelvic floor and abdominal muscles in women with and without incontinence. Neurourol Urodyn. 2007;26:377–85. https://doi.org/ 10.1002/nau.20336.
Stuge B, Mørkved S, Dahl HH, Vøllestad N. Abdominal and pelvic floor muscle function in women with and without long lasting pelvic girdle pain. Man Ther. 2006;211(4):287–96. https://doi.org/10. 1016/j.math.2005.07.003.
Sjödahl J, Gutke A, Ghaffari G, et al. Response of the muscles in the pelvic floor and the lower lateral abdominal wall during the active straight leg raise in women with and without pelvic girdle pain: an experimental study. Clin Biomech Bristol Avon. 2016;35: https://doi.org/10.1016/j.clinbiomech.2016.04.007.
Bi X, Zhao J, Zhao L, et al. Pelvic floor muscle exercise for chroniclow back pain. J Int Med Res. 2013;41:146–52.https://doi.org/10.1177/0300060513475383.51. ElDeeb AM, Abd-Ghafar KS, Ayad WA, Sabbour AA. Effect of segmental stabilizing exercises augmented by pelvic floor musclestraining on women with postpartum pelvic girdle pain: a random-ized controlled trial. J Back Musculoskelet Rehabil. 2019;32:693–700.https://doi.org/10.3233/BMR-181258.52.
Ghaderi F, Mohammadi K, Amir Sasan R, et al. Effects of stabili-zation exercises focusing on pelvic floor muscles on low back painand urinary incontinence in women. Urology. 20 16;93:50–4.https://doi.org/10.1016/j.urology.2016.03.034.53.
Teymuri Z, Hosseinifar M, Sirousi M. The effect of stabilization exercises on pain, disability, and pelvic floor muscle function inpostpartum lumbopelvic pain: a randomized controlled trial. Am JPhys Med Rehabil. 2018;97:885–91.https://doi.org/10.1097/PHM.0000000000000993.54.
Taylor DA, Merten SL, Sandercoe GD, Gahankari D, Ingram SB,Moncrieff NJ, et al. Abdominoplasty improves low back pain andurinary incontinence. Plast Reconstr Surg. 2018;141(3):637–45.https://doi.org/10.1097/PRS.0000000000004100